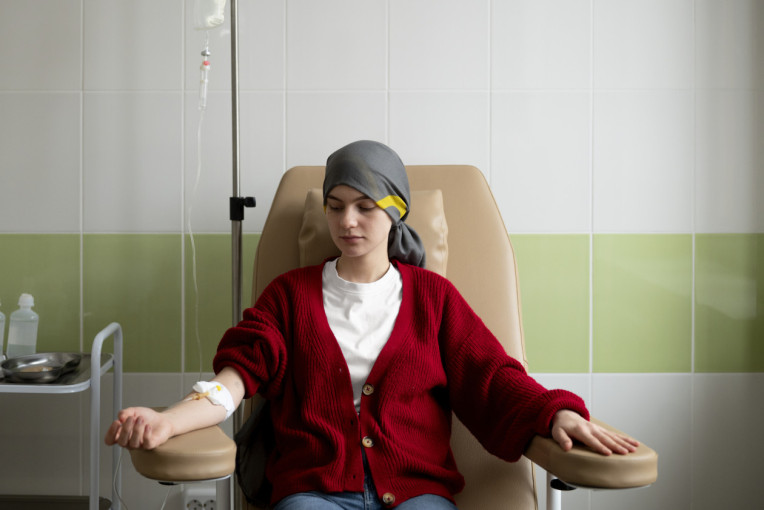
Ramadan is a deeply meaningful time for Muslims, including patients undergoing cancer treatment. The desire to continue fasting arises as part of spiritual strengthening, while medical conditions and immune resilience during treatment require careful consideration, chemotherapy and radiotherapy can affect nutritional intake, hydration, and daily stamina. Therefore, the decision to fast should be based on a comprehensive clinical evaluation.
A surgical oncologist at Universitas Gadjah Mada Academic Hospital (RSA UGM), Dr. R. Wahyu Kartiko Tomo, explained that the decision to fast for cancer patients is highly individualized. He emphasized that not all patients are automatically prohibited from observing Ramadan fasting.
Medical assessments must take into account the type of cancer, stage of disease, nutritional status, and ongoing therapies. Comorbidities such as diabetes, kidney disorders, or heart problems are also important factors in making this decision.
“In general, whether fasting is permissible depends on each patient’s clinical condition,” he said on Monday (Feb. 23).
According to Dr. Tomo, as he is fondly known, the main principle in determining eligibility for fasting is ensuring that it does not interfere with the effectiveness of therapy. If fasting has the potential to worsen the condition or hinder treatment, it should be postponed.
He stressed that patient safety remains the top priority in any medical decision. A thorough evaluation prior to Ramadan is strongly recommended so patients understand the potential risks.
“The principle is that if fasting could disrupt therapy or worsen the clinical condition, it should be postponed,” he explained.
Dr. Tomo further noted that chemotherapy often causes side effects such as nausea, vomiting, loss of appetite, and severe fatigue. The risk of dehydration and electrolyte imbalance may also increase during treatment.
With limited fluid and calorie intake, fasting can exacerbate these symptoms. Patients with poor nutritional status require special attention, as they are more vulnerable to rapid weight loss.
“Fasting may further exacerbate the condition, especially if fluid intake is insufficient and calorie intake is inadequate,” he said.
Dr. Tomo added that radiotherapy also presents specific challenges depending on the area being treated. Radiation to the head and neck can cause painful swallowing and difficulty eating. Radiation to the abdominal area may trigger nausea or diarrhea, while exposure to large areas often results in severe fatigue.
In such situations, limiting intake during fasting may increase the risk of dehydration and significant weight loss. These conditions could disrupt the continuation of therapy if not properly managed.
“In such circumstances, fasting may increase the risk of dehydration and significant weight loss,” he stated.
He added that certain groups of patients are generally not advised to fast. Patients with advanced-stage cancer accompanied by poor general condition, cachexia, or severe malnutrition require special consideration.
Those undergoing intensive chemotherapy during early cycles or experiencing complications such as severe infections or kidney disorders should also consider postponing fasting.
The decision is not based solely on the stage of cancer, but rather on overall clinical status and physical resilience.
“It is not merely about the stage, but about the clinical condition and the body’s resilience,” Dr. Tomo said.
Potential risks for patients who insist on fasting include dehydration, hypoglycemia, electrolyte imbalance, and rapid weight loss. Severe fatigue and worsening kidney function may also occur in certain conditions.
In some cases, Dr. Tomo noted, these complications can lead to delays in therapy cycles. Postponed treatment may affect the overall effectiveness of cancer management.
“In some cases, this can impact treatment effectiveness,” he said.
Nevertheless, patients with stable conditions may still have the opportunity to fast under medical supervision. Dr. Tomo recommends clinical evaluation before Ramadan and consultation for possible medication schedule adjustments.
A minimum fluid intake of 1.5 – 2 liters between iftar and sahur (pre-dawn meal before fasting) is advised, if the condition allows, along with high-calorie and high-protein foods. Patients may also fast on alternate days according to their tolerance and should break the fast immediately if severe symptoms arise.
“Fasting is a noble act of worship, but safeguarding health and preserving life are also acts of worship,” he concluded.
Author: Triya Andriyani
Post-editor: Jasmine Ferdian
Photo: Freepik

